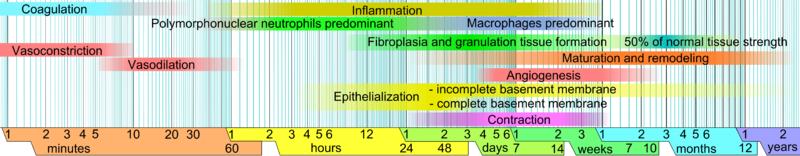
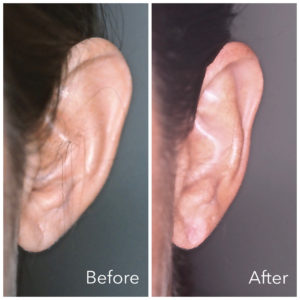
Successful wound healing occurs when the outcome of an injury or surgical procedure is a minimally apparent scar. Many variables can affect the final result of wound healing, including the size and depth of the wound, the blood supply to the area, the thickness and color of your skin, and tension on the repair. There are three principal phases in the wound healing process: inflammation, transitional repair, and maturation.
Inflammation Phase
The healing process begins immediately following tissue injury when blood vessels begin to narrow and clot, releasing various chemical substances into the wound. The extent of wound inflammation that is produced can be affected by the length of time that passes until the wound is repaired.
Transitional Repair Phase
During the transitional repair phase the density of cells in the tissue around the wound increase, beginning several days after the injury and lasting for several weeks. New skin cells and blood vessels begin to form to maximize the tissue replacement. These new blood vessels will supply the rebuilding cells with oxygen and nutrients to sustain the growth of the new cells and support the production of collagen, which acts as the framework for wound repair.
Maturation Phase
Scar maturation begins within 6-12 weeks and is the final phase of wound healing. This phase produces an improved scar contour as the collagen remodels from type III to type I. Less redness of the scar results from reduced cellular activity and a decrease in the number of blood vessels.
There are two different types of unfavorable scars that can appear after a surgical procedure. A hypertrophic scar is a thick, disfiguring scar that is usually raised above the skin surface. It can be caused by prolonged inflammation of the wound due to infection or excessive tension on the wound repair. This type of thickened scar will often improve over time. A keloid scar is an outcome of healing that results from a genetic predisposition to forming a thickened mass of scar tissue extending beyond the borders of the original wound. It generally does not regress and frequently resists attempts at treatment.
Our next blog will discuss techniques for managing surgical scars to get the most favorable result.
Tags: Plastic Surgery, scars, wound healing
Written by Dr. Forley on December 31, 2012